Every year, World Diabetes Day reminds us that diabetes is not just about blood sugar — it’s also about protecting the skin and wounds that often go unnoticed. For people living with diabetes, a small cut can turn into a serious infection if not properly cared for. According to the Centers for Disease Control and Prevention (CDC), about 15% of people with diabetes will develop a diabetic foot ulcer in their lifetime, and infections from these ulcers lead to up to 85% of diabetes-related amputations.
Why Wounds Heal Differently in People with Diabetes
Diabetes affects wound healing on multiple levels. High blood glucose can narrow blood vessels and reduce circulation, making it harder for oxygen and nutrients to reach damaged tissue. The immune system also becomes less effective, slowing down the body’s natural ability to fight infection and rebuild skin.
A 2023 study in Diabetes Care found that chronic hyperglycemia reduces collagen synthesis by up to 50%, weakening new tissue formation and leading to delayed healing. Additionally, diabetic neuropathy — nerve damage caused by long-term high blood sugar — can reduce sensation, meaning many patients don’t feel pain or notice small wounds until they become serious.
The Hidden Dangers: Everyday Wounds That Become Complicated
Simple blisters, pressure spots, or insect bites can quickly become problematic for diabetic patients. Common areas of concern include the feet, heels, and lower legs, where circulation is naturally weaker. The American Diabetes Association (ADA) reports that roughly 20% of diabetic patients admitted to hospitals have an active foot ulcer or infection.
Without timely care, these wounds can develop into chronic ulcers or deep tissue infections. Once bacteria penetrate the skin, biofilm formation can occur — a protective layer that makes bacteria up to 1,000 times more resistant to antibiotics and antiseptics (Wound Repair and Regeneration, 2022).
Smart Wound Care for Diabetic Skin
Clean and Protect
The first step in diabetic wound care is gentle cleansing. Avoid alcohol-based antiseptics that can dry or damage the skin barrier. Instead, use sterile saline or mild wound cleansers to remove debris without irritating healthy tissue.
After cleaning, apply a protective dressing that maintains a moist environment — essential for optimal healing. Hydrocolloid or hydrogel dressings are ideal for mild to moderate exudate wounds, helping retain moisture while promoting autolytic debridement (natural removal of dead tissue).
Watch for Signs of Infection
Check wounds daily for any changes in color, odor, or swelling. Even minor redness or warmth may indicate infection. Diabetic patients should be especially cautious — infections can spread quickly. If a wound isn’t improving within 7–10 days, seek medical attention.
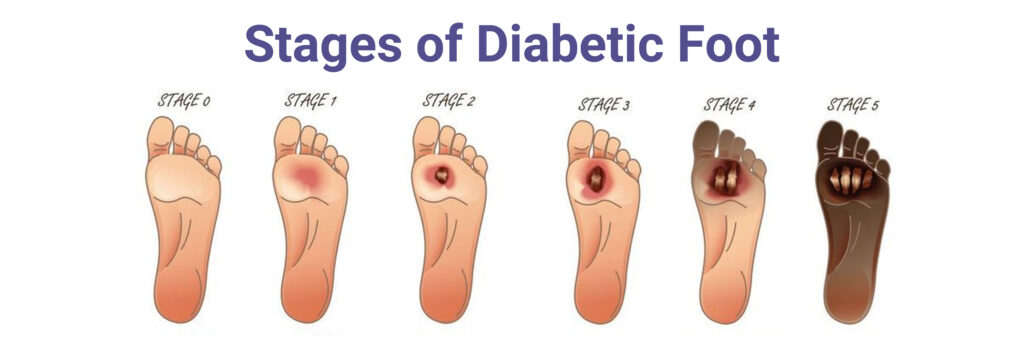
Choose Advanced Wound Dressings
When it comes to diabetic wound management, choosing the right dressing can make a real difference.
Two proven options are ConkoAlgi Ag (silver alginate dressing) and ConkoSil (silicone foam dressing):
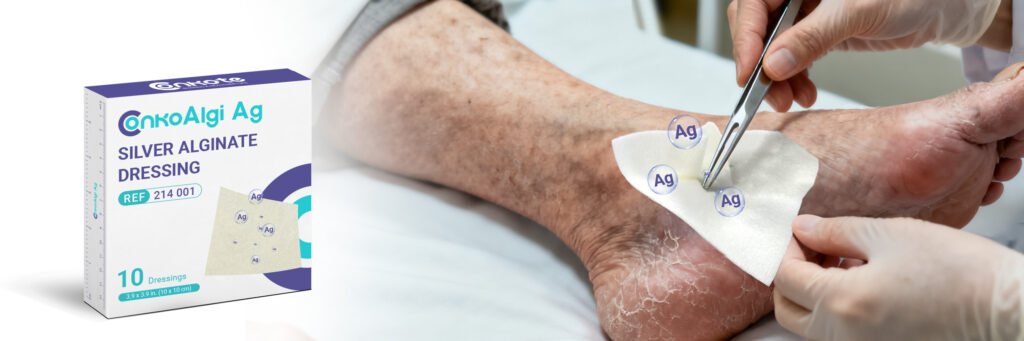
- ConkoAlgi Ag (silver alginate dressing)
Made from natural silver alginate — a blend of alginate fibers derived from seaweed and silver ions — these dressings form a soft gel upon contact with wound exudate. This gel structure conforms closely to the wound bed, keeping the area moist and comfortable while promoting autolytic debridement. The presence of silver ions provides strong antibacterial protection, effectively reducing the growth of a wide range of pathogens. This combination helps maintain an optimal healing environment and supports faster, safer recovery for diabetic wounds.
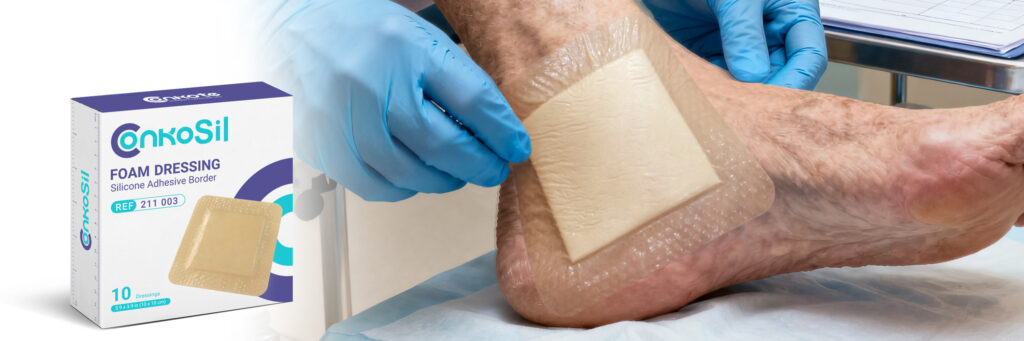
- ConkoSil (silicone foam dressing):
Ideal for fragile or sensitive diabetic skin, silicone foam provides gentle adhesion and painless removal. The soft silicone border protects against friction and pressure — two major causes of delayed healing in diabetic foot ulcers.
These modern wound care materials help prevent infection, manage exudate, and support the natural healing process — all crucial for diabetic patients with compromised skin integrity.
Keep Pressure Off
Reducing pressure on the wound is crucial, especially for diabetic foot ulcers. Offloading techniques such as special footwear, foam padding, or dressings with built-in cushioning help prevent friction and promote faster recovery.
Prevention Is the Best Cure
Daily foot inspection, regular moisturizing, and early treatment of small wounds can significantly reduce complications. According to a BMJ Open Diabetes Research & Care review (2024), preventive care and early intervention can reduce diabetic amputation rates by up to 49%.
Maintaining stable blood sugar levels, wearing breathable footwear, and avoiding walking barefoot all play a part in wound prevention. For healthcare providers and caregivers, patient education remains the most powerful tool — awareness can literally save limbs.
Takeaway
This World Diabetes Day, let’s not just talk about controlling sugar — let’s talk about protecting the skin.
Healthy skin is the body’s first defense, and for those with diabetes, it’s also a vital part of long-term health and independence.
At Conkote, we believe in smarter healing — supporting every stage of diabetic wound care with reliable protection and innovation. Because healing should never be left to chance.



