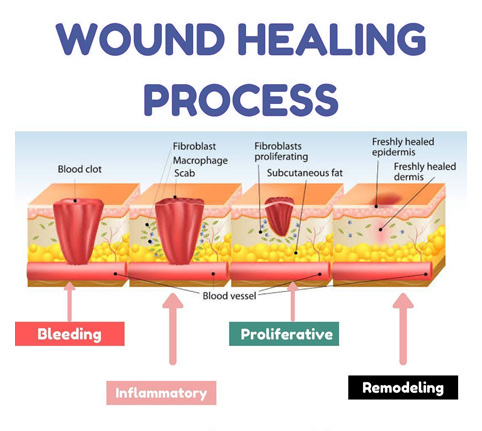
Understanding how a wound heals is essential for choosing the right care at the right time. Many people assume that once a wound stops bleeding or forms a scab, healing is complete. In reality, wound healing is a complex, biological process that unfolds in four distinct stages, each with its own purpose and care priorities.
By understanding these stages, patients, caregivers, and healthcare professionals can make better decisions that support natural healing and reduce the risk of complications.
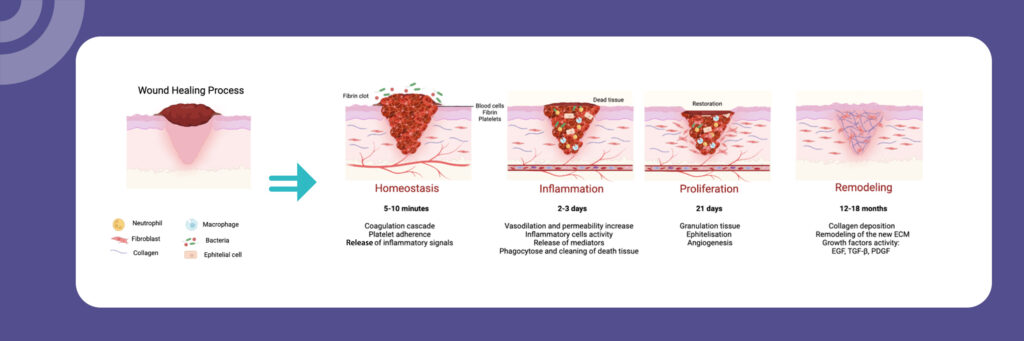
Stage 1: Hemostasis – Stopping the Bleeding
When it happens: Immediately after injury, lasting minutes to hours
Hemostasis is the body’s first response to injury. Its primary goal is simple but critical: to stop bleeding.
During this stage:
- Blood vessels constrict to reduce blood flow
- Platelets gather at the wound site
- A clot forms to seal the damaged tissue
This clot acts as a temporary protective barrier, helping prevent excessive blood loss and reducing exposure to external contaminants.
Care considerations at this stage:
- Keep the wound clean and protected
- Avoid unnecessary disturbance of the clot
- Do not change dressings too frequently unless bleeding continues
Proper initial coverage helps create a stable foundation for the next stages of healing.
Stage 2: Inflammation – Cleaning and Defending
When it happens: Within hours of injury, lasting several days
Inflammation is often misunderstood. Redness, warmth, swelling, and mild pain are not signs of failure—they are signs that the body’s defense system is working.
During this stage:
- White blood cells migrate to the wound
- Bacteria and debris are broken down
- Damaged tissue is removed to prepare for repair
A controlled inflammatory response is essential for healing. However, excessive or prolonged inflammation may indicate infection or delayed recovery.
Care considerations at this stage:
- Monitor the wound for changes in pain, odor, or drainage
- Manage excess exudate to protect surrounding skin
- Reduce infection risk without overusing harsh antiseptics
Dressings that help control moisture and protect the wound environment can play an important role during this phase.
Stage 3: Proliferation – Building New Tissue
When it happens: Typically begins a few days after injury and can last weeks
This is the stage where visible healing truly begins. The body starts rebuilding what was lost.
During proliferation:
- New granulation tissue forms
- Blood vessels regenerate to supply oxygen and nutrients
- The wound edges begin to contract
- New epithelial cells migrate across the wound surface
A balanced, moist wound environment is especially important at this stage. Too much dryness can slow cell migration, while excess moisture may damage fragile new tissue.
Care considerations at this stage:
- Maintain a moist but controlled wound environment
- Protect newly formed tissue from friction and trauma
- Use dressings that minimize pain and disruption during changes
Supporting this stage properly helps promote steady progress toward closure.
Stage 4: Maturation (Remodeling) – Strengthening the Skin
When it happens: Begins once the wound is closed and may last months
Although the wound may appear healed, the body continues working beneath the surface.
During maturation:
- Collagen fibers reorganize and strengthen
- Blood supply to the area decreases
- Scar tissue gradually becomes more flexible
The repaired skin may only regain 70–80% of its original strength, making it more vulnerable to re-injury.
Care considerations at this stage:
- Protect the area from excessive pressure or friction
- Support fragile skin as it adapts
- Pay attention to scar management when appropriate
Gentle, supportive care during this phase helps preserve long-term skin integrity.
Common Misunderstandings About Wound Healing
Despite growing awareness, several myths still persist:
- “A dry scab means faster healing.” In many cases, overly dry wounds heal more slowly.
- “Redness always means infection.” Some redness is a normal part of inflammation.
- “All wounds need the same type of dressing.” Different stages require different approaches.
- “Once pain is gone, care is no longer needed.” Healing continues long after discomfort fades.
Recognizing these misconceptions can prevent setbacks and unnecessary complications.
Why Understanding the Healing Stages Matters
Wound healing is not a straight line. It is a dynamic process that responds to local conditions, overall health, and daily care decisions.
By understanding the four stages of wound healing, caregivers and patients can:
- Respond appropriately to normal changes
- Identify warning signs earlier
- Choose care strategies that align with the wound’s current needs
Supporting the body’s natural healing process at each stage leads to safer, more effective recovery and better long-term outcomes.