Chronic pressure ulcers (PUs), also known as bedsores, are common among elderly and immobile patients. They develop when prolonged pressure on the skin reduces blood flow, leading to tissue damage. Pressure ulcers can result in infections, delayed healing, and decreased quality of life.
Proper dressing care, combined with holistic wound management, is essential to accelerate healing and prevent complications. Evidence shows that selecting the right dressing significantly improves recovery outcomes (Verywell Health, 2025).
Understanding Pressure Ulcer Stages
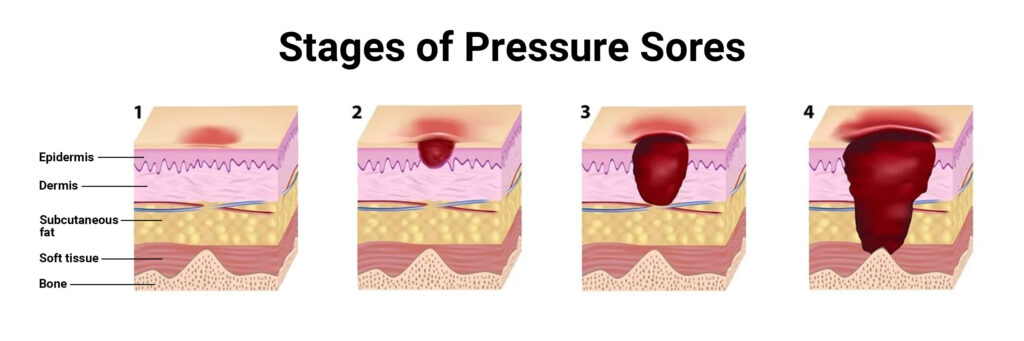
Pressure ulcers are classified into four stages:
- Stage 1: Intact skin with persistent redness over a bony area.
- Stage 2: Partial-thickness loss of dermis, presenting as a shallow open ulcer.
- Stage 3: Full-thickness tissue loss with visible subcutaneous fat (bone/muscle not exposed).
- Stage 4: Full-thickness tissue loss with exposed bone, tendon, or muscle. Slough or eschar may be present.
Additionally:
- Unstageable: Wound base is obscured by slough or eschar.
- Deep Tissue Pressure Injury: Discolored intact skin or blood-filled blister from underlying tissue damage (Verywell Health, 2025).
Causes and Risk Factors

Pressure ulcers result from prolonged pressure and shear that compromise blood flow. Key risk factors include:
- Immobility: Limited ability to change positions (Homerton NHS)
- Incontinence: Prolonged exposure to moisture from urine or stool (Mayo Clinic)
- Poor nutrition: Insufficient protein, vitamins, and calories
- Age: Thinner skin and less subcutaneous tissue in older adults
- Medical conditions: Diabetes, vascular diseases, neurological disorders
Understanding these factors helps in both prevention and effective management.
From Risk Awareness to Practical Care
While immobility, incontinence, poor nutrition, and chronic diseases increase the risk of pressure ulcers, identifying these factors is only the first step. To effectively prevent and heal chronic wounds, caregivers must implement targeted, evidence-based care strategies that directly address these risks. The following approaches provide practical guidance for everyday wound management, supporting both healing and patient comfort.
Comprehensive Wound Care Strategies
- Regular Repositioning:
- Turn or reposition patients every 2 hours to relieve pressure on bony areas.
- Studies show consistent repositioning reduces the risk of new pressure ulcers by up to 50%.
- Targeted Nutritional Support:
- Provide adequate protein, vitamins C and A, and zinc to promote tissue repair.
- Malnourished patients take significantly longer to heal wounds.
- Debridement and Cleaning:
- Gently remove necrotic tissue to encourage granulation.
- Use sterile techniques to reduce infection risk.
- Combine with dressings that support autolytic debridement.
- Moisture & Infection Control:
- Keep surrounding skin clean and dry to prevent maceration.
- Monitor for infection: redness, foul odor, increased exudate.
- Advanced dressings like silver-ion or hydrocolloid can actively reduce microbial load.
- Patient & Caregiver Education:
- Teach proper turning techniques, skin inspection, and dressing changes.
- Educated caregivers improve adherence and speed up recovery.
Moisture Management & Dressing Solutions
Maintaining a moist wound environment is essential for healing chronic pressure ulcers. Conkote provides three advanced dressing options to meet different wound care needs, each designed to support moisture balance and optimize healing.
 |  |  | |
| Product | Foam Dressing Silicone Adhesive Border | Hydrocolloid Dressing | Silver Alginate Dressing |
| Function | Absorbs exudate, cushions wound, minimizes trauma during dressing changes | Creates a moist healing environment | Antimicrobial, prevents infection |
| Application | Moderate to heavily exuding wounds; maintains moist environment for faster healing | Suitable for shallow or stage 2 wounds; promotes autolytic debridement and protects surrounding skin | Perfect for infected or high-risk wounds; maintains a moist environment while reducing bacterial load |
Patient Education and Engagement
Educating patients and caregivers improves adherence:
- Teach proper dressing application and monitoring.
- Identify infection signs and when to seek medical help.
- Encourage lifestyle adjustments, including nutrition and mobility.
Conclusion
Chronic pressure ulcers require a multi-faceted management approach:
- Use evidence-based dressings tailored to the wound stage.
- Maintain optimal moisture levels to support tissue repair.
- Implement holistic wound care strategies including nutrition, repositioning, and infection control.
- Educate patients and caregivers to enhance adherence and healing.
By integrating these practices, healthcare providers can improve healing outcomes, reduce complications, and enhance quality of life for patients with chronic pressure ulcers.


